Wij zijn ons brein, schreef een hersenwetenschapper. Wij zijn onze hormonen, schreef een endocrinoloog. Allebei waar, maar we worden ook deels aangestuurd door ‘beestjes’ in onze darmen.
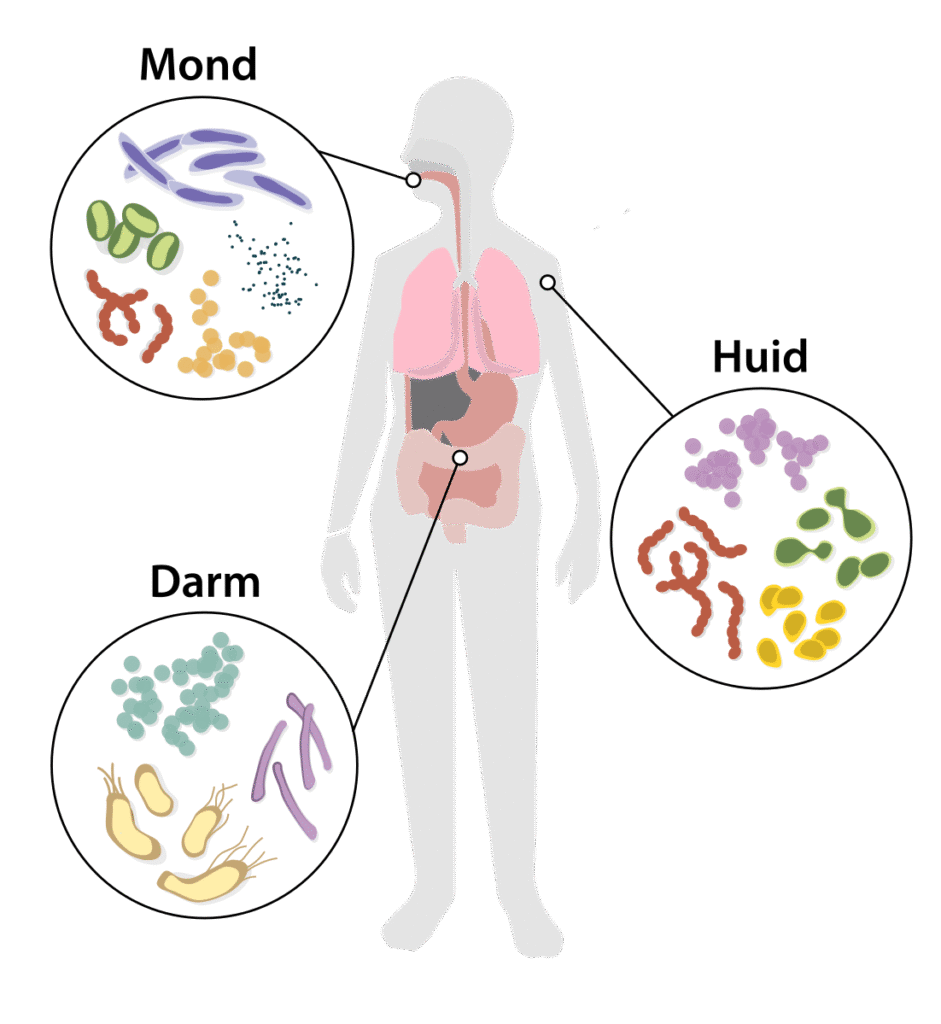
Overal waar ons lichaam grenst aan de omgeving, zoals de huid, longen, urineweg en sommige klieren, zoals de borst-, prostaat en alvleesklier, wonen microben: bacteriën, virussen, schimmels en parasieten.
Het aantal bacteriën in en op ons lichaam is enorm. Met 30 tot 40 biljoen bacteriën zijn het er net zoveel als het totaal aantal cellen waaruit we zijn opgebouwd. Verreweg het grootste aantal woont in ons maagdarmkanaal, vooral onze dikke darm. Deze micro-organismen tezamen heten onze ‘microbiota’. Het ‘microbioom’ omvat al hun genen en producten. Ons darm-microbioom beschikt over 130 keer meer genen dan wijzelf. Overdonderende getallen die de vraag oproepen wie wij eigenlijk zijn. Het antwoord is dat wij een eenheid vormen met onze microbiota. We kunnen niet zonder elkaar en als we ze slecht behandelen gaat het mis. Zo vertonen proefdieren die zonder microbiota opgroeien onder andere abnormaal (sociaal) gedrag.
De microbiota beïnvloedt ons door contact met hun celwand en stoffen die ze uitscheiden. Veel daarvan zijn nuttig, zoals korteketenvetzuren, vitamines, hormonen en (valse) neurotransmitters, maar andere zijn ongunstig voor ons. Op deze manier beïnvloeden ze bijvoorbeeld onze darmbewegingen, wat kan leiden tot diarree, verstopping en pijn. Wat je eet, bepaalt in sterke mate hun samenstelling. Een veranderd voedingspatroon is binnen 24 uur zichtbaar in een aangepast darm-microbioom. Ook factoren als genetische achtergrond, of je vaginaal dan wel via een keizersnede bent geboren, en of je borstvoeding hebt gehad, spelen een rol. Daarnaast wordt het darm-microbioom beïnvloed door leeftijd, geslacht, hoeveel je beweegt, stress en antibioticagebruik.
Deels zijn wij marionetten aan de touwtjes van onze microbiota
Wie goed voor zijn microbioom zorgt, zorgt goed voor zichzelf. Een evenwichtig microbioom heeft een positieve invloed op nagenoeg al onze organen, systemen en functies, zoals de hersenen, ons immuunsysteem, en de barrière in onze darmen. Het gezondste microbioom is zo divers mogelijk van samenstelling. Je verkrijgt het door een voeding die relatief veel groente en fruit, en dus veel vezels, bevat. Vóór de gemengde landbouw-veeteelt revolutie – ongeveer 10.000 jaar geleden – was de microbioom-diversiteit in onze mondholte veel groter dan nu. Traditioneel levende bevolkingen hebben een diverser darm-microbioom dan wij.
Onze hersenen en darm communiceren voortdurend met elkaar via de microbiota-darm-hersen-as. Deels fungeren onze darmen als een autonoom centrum. Daarom worden ze ook wel ons ‘tweede brein’ genoemd. Via deze communicatiewegen wordt de microbiota geassocieerd met het ontstaan van angst en stress, verslaving, pijn, neurodegeneratieve ziektes zoals MS, Alzheimer, Parkinson, maar ook autisme, schizofrenie, boezemfibrilleren en chronische ontstekingen van de darmen (ziekte van Crohn, colitis ulcerosa). Het prikkelbare darmsyndroom is het prototype van een verstoorde microbiota-darm-hersen-as, maar ook autisme wordt als zo’n verstoring gezien. Ratten die via transplantatie de microbiota van depressieve personen ontvangen vertonen daarna ook depressief gedrag. Niet zelden is hierbij sprake van een ‘lekkende darm’, een conditie die ervoor zorgt dat stoffen uit onze darmen de bloedbaan gemakkelijker bereiken.
De microbiota beïnvloedt ook ons eetgedrag en kan op die manier leiden tot obesitas, metabool syndroom en diabetes mellitus type 2. Dat doen ze via het stimuleren van onze beloningssystemen, beïnvloeding van de stemming, verandering van smaakreceptoren en het prikkelen van zenuwen die signalen naar de hersenen sturen. We zijn dus deels marionetten aan de touwtjes van ons darm-microbioom. Krijg je ‘trek’ in eten? Bedenk dan wie er nu eigenlijk honger heeft…
Beeld: Wikimedia Commons
1. Hill JH, Round JL. SnapShot: Microbiota effects on host physiology. Cell. 2021 May 13;184(10):2796-2796.e1. doi: 10.1016/j.cell.2021.04.026. PMID: 33989551.
https://pubmed.ncbi.nlm.nih.gov/33989551
2. Hartstra AV, Bouter KE, Bäckhed F, Nieuwdorp M. Insights into the role of the microbiome in obesity and type 2 diabetes. Diabetes Care. 2015 Jan;38(1):159-65. doi: 10.2337/dc14-0769. PMID: 25538312.
https://pubmed.ncbi.nlm.nih.gov/25538312
2a. Mowat AM, Agace WW. Regional specialization within the intestinal immune system. Nat Rev Immunol. 2014 Oct;14(10):667-85. doi: 10.1038/nri3738. Epub 2014 Sep 19. PMID: 25234148.
https://pubmed.ncbi.nlm.nih.gov/25234148
3. Sender R, Fuchs S, Milo R. Revised Estimates for the Number of Human and Bacteria Cells in the Body. PLoS Biol. 2016 Aug 19;14(8):e1002533. doi: 10.1371/journal.pbio.1002533. PMID: 27541692; PMCID: PMC4991899.
https://pubmed.ncbi.nlm.nih.gov/27541692
3a. Gilbert JA, Blaser MJ, Caporaso JG, Jansson JK, Lynch SV, Knight R. Current understanding of the human microbiome. Nat Med. 2018 Apr 10;24(4):392-400. doi: 10.1038/nm.4517. PMID: 29634682; PMCID: PMC7043356.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7043356
4. Sender R, Fuchs S, Milo R. Are We Really Vastly Outnumbered? Revisiting the Ratio of Bacterial to Host Cells in Humans. Cell. 2016 Jan 28;164(3):337-40. doi: 10.1016/j.cell.2016.01.013. PMID: 26824647.
https://pubmed.ncbi.nlm.nih.gov/26824647
5. Zhao L. The gut microbiota and obesity: from correlation to causality. Nat Rev Microbiol. 2013 Sep;11(9):639-47. doi: 10.1038/nrmicro3089. Epub 2013 Aug 5. PMID: 23912213.
https://pubmed.ncbi.nlm.nih.gov/23912213
5a. Wallace CJK, Milev R. The effects of probiotics on depressive symptoms in humans: a systematic review. Ann Gen Psychiatry. 2017 Feb 20;16:14. doi: 10.1186/s12991-017-0138-2. Erratum in: Ann Gen Psychiatry. 2017 Mar 7;16:18. doi: 10.1186/s12991-017-0141-7. PMID: 28239408; PMCID: PMC5319175.
https://pubmed.ncbi.nlm.nih.gov/28239408
5b. Lagier JC, Million M, Hugon P, Armougom F, Raoult D. Human gut microbiota: repertoire and variations. Front Cell Infect Microbiol. 2012 Nov 2;2:136. doi: 10.3389/fcimb.2012.00136. PMID: 23130351; PMCID: PMC3487222.
https://pubmed.ncbi.nlm.nih.gov/23130351
5c. Varghese S, Rao S, Khattak A, Zamir F, Chaari A. Physical Exercise and the Gut Microbiome: A Bidirectional Relationship Influencing Health and Performance. Nutrients. 2024 Oct 28;16(21):3663. doi: 10.3390/nu16213663. PMID: 39519496; PMCID: PMC11547208.
https://pubmed.ncbi.nlm.nih.gov/39519496
5d. Scott KP, Gratz SW, Sheridan PO, Flint HJ, Duncan SH. The influence of diet on the gut microbiota. Pharmacol Res. 2013 Mar;69(1):52-60. doi: 10.1016/j.phrs.2012.10.020. Epub 2012 Nov 9. PMID: 23147033.
5e. Lim ES, Wang D, Holtz LR. The Bacterial Microbiome and Virome Milestones of Infant Development. Trends Microbiol. 2016 Oct;24(10):801-810. doi: 10.1016/j.tim.2016.06.001. Epub 2016 Jun 25. PMID: 27353648.
https://pubmed.ncbi.nlm.nih.gov/27353648
5f. Lim ES, Wang D, Holtz LR. The Bacterial Microbiome and Virome Milestones of Infant Development. Trends Microbiol. 2016 Oct;24(10):801-810. doi: 10.1016/j.tim.2016.06.001. Epub 2016 Jun 25. PMID: 27353648.
https://pubmed.ncbi.nlm.nih.gov/27353648
5g. Lambrecht BN, Hammad H. The immunology of the allergy epidemic and the hygiene hypothesis. Nat Immunol. 2017 Sep 19;18(10):1076-1083. doi: 10.1038/ni.3829. PMID: 28926539.
https://pubmed.ncbi.nlm.nih.gov/28926539
5h. Paliy O, Piyathilake CJ, Kozyrskyj A, Celep G, Marotta F, Rastmanesh R. Excess body weight during pregnancy and offspring obesity: potential mechanisms. Nutrition. 2014 Mar;30(3):245-51. doi: 10.1016/j.nut.2013.05.011. Epub 2013 Oct 6. PMID: 24103493.
https://pubmed.ncbi.nlm.nih.gov/24103493
https://pubmed.ncbi.nlm.nih.gov/23147033
6. Ley RE, Hamady M, Lozupone C, Turnbaugh PJ, Ramey RR, Bircher JS, Schlegel ML, Tucker TA, Schrenzel MD, Knight R, Gordon JI. Evolution of mammals and their gut microbes. Science. 2008 Jun 20;320(5883):1647-51. doi: 10.1126/science.1155725. Epub 2008 May 22. Erratum in: Science. 2008 Nov 21;322(5905):1188. PMID: 18497261; PMCID: PMC2649005.
https://pubmed.ncbi.nlm.nih.gov/18497261
7. Fackelmann G, Manghi P, Carlino N, Heidrich V, Piccinno G, Ricci L, Piperni E, Arrè A, Bakker E, Creedon AC, Francis L, Capdevila Pujol J, Davies R, Wolf J, Bermingham KM, Berry SE, Spector TD, Asnicar F, Segata N. Gut microbiome signatures of vegan, vegetarian and omnivore diets and associated health outcomes across 21,561 individuals. Nat Microbiol. 2025 Jan;10(1):41-52. doi: 10.1038/s41564-024-01870-z. Epub 2025 Jan 6. PMID: 39762435; PMCID: PMC11726441.
https://pubmed.ncbi.nlm.nih.gov/39762435
8. Whiteside SA, Razvi H, Dave S, Reid G, Burton JP. The microbiome of the urinary tract–a role beyond infection. Nat Rev Urol. 2015 Feb;12(2):81-90. doi: 10.1038/nrurol.2014.361. Epub 2015 Jan 20. PMID: 25600098.
https://pubmed.ncbi.nlm.nih.gov/25600098
9. Rook G, Bäckhed F, Levin BR, McFall-Ngai MJ, McLean AR. Evolution, human-microbe interactions, and life history plasticity. Lancet. 2017 Jul 29;390(10093):521-530. doi: 10.1016/S0140-6736(17)30566-4. Epub 2017 Jul 27. PMID: 28792414.
https://pubmed.ncbi.nlm.nih.gov/28792414
Microbiota diversity and ancient microbiota
9ax. Mosca A, Leclerc M, Hugot JP. Gut Microbiota Diversity and Human Diseases: Should We Reintroduce Key Predators in Our Ecosystem? Front Microbiol. 2016 Mar 31;7:455. doi: 10.3389/fmicb.2016.00455. PMID: 27065999; PMCID: PMC4815357.
https://pubmed.ncbi.nlm.nih.gov/27065999
9b. Grace-Farfaglia P, Frazier H, Iversen MD. Essential Factors for a Healthy Microbiome: A Scoping Review. Int J Environ Res Public Health. 2022 Jul 8;19(14):8361. doi: 10.3390/ijerph19148361. PMID: 35886216; PMCID: PMC9315476.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9315476
9c. Schnorr SL. The diverse microbiome of the hunter-gatherer. Nature. 2015 Feb 26;518(7540):S14-5. doi: 10.1038/518S14a. PMID: 25715276.
https://pubmed.ncbi.nlm.nih.gov/25715276
9d. Rampelli S, Schnorr SL, Consolandi C, Turroni S, Severgnini M, Peano C, Brigidi P, Crittenden AN, Henry AG, Candela M. Metagenome Sequencing of the Hadza Hunter-Gatherer Gut Microbiota. Curr Biol. 2015 Jun 29;25(13):1682-93. doi: 10.1016/j.cub.2015.04.055. Epub 2015 May 14. PMID: 25981789.
https://pubmed.ncbi.nlm.nih.gov/25981789
9e. Moeller AH, Li Y, Mpoudi Ngole E, Ahuka-Mundeke S, Lonsdorf EV, Pusey AE, Peeters M, Hahn BH, Ochman H. Rapid changes in the gut microbiome during human evolution. Proc Natl Acad Sci U S A. 2014 Nov 18;111(46):16431-5. doi: 10.1073/pnas.1419136111. Epub 2014 Nov 3. PMID: 25368157; PMCID: PMC4246287.
https://pubmed.ncbi.nlm.nih.gov/25368157
10. Alcock J, Maley CC, Aktipis CA. Is eating behavior manipulated by the gastrointestinal microbiota? Evolutionary pressures and potential mechanisms. Bioessays. 2014 Oct;36(10):940-9. doi: 10.1002/bies.201400071. Epub 2014 Aug 8. PMID: 25103109; PMCID: PMC4270213.
https://pubmed.ncbi.nlm.nih.gov/25103109
11. Wu GD, Chen J, Hoffmann C, Bittinger K, Chen YY, Keilbaugh SA, Bewtra M, Knights D, Walters WA, Knight R, Sinha R, Gilroy E, Gupta K, Baldassano R, Nessel L, Li H, Bushman FD, Lewis JD. Linking long-term dietary patterns with gut microbial enterotypes. Science. 2011 Oct 7;334(6052):105-8. doi: 10.1126/science.1208344. Epub 2011 Sep 1. PMID: 21885731; PMCID: PMC3368382.
https://pubmed.ncbi.nlm.nih.gov/21885731
12. Flint HJ, Scott KP, Louis P, Duncan SH. The role of the gut microbiota in nutrition and health. Nat Rev Gastroenterol Hepatol. 2012 Sep 4;9(10):577-89. doi: 10.1038/nrgastro.2012.156. PMID: 22945443.
https://pubmed.ncbi.nlm.nih.gov/22945443
13. Turnbaugh PJ, Ley RE, Hamady M, Fraser-Liggett CM, Knight R, Gordon JI. The human microbiome project. Nature. 2007 Oct 18;449(7164):804-10. doi: 10.1038/nature06244. PMID: 17943116; PMCID: PMC3709439.
https://pubmed.ncbi.nlm.nih.gov/17943116
14. Wu G, Xu T, Zhao N, Lam YY, Ding X, Wei D, Fan J, Shi Y, Li X, Li M, Ji S, Wang X, Fu H, Zhang F, Shi Y, Zhang C, Peng Y, Zhao L. A core microbiome signature as an indicator of health. Cell. 2024 Nov 14;187(23):6550-6565.e11. doi: 10.1016/j.cell.2024.09.019. Epub 2024 Oct 7. PMID: 39378879.
https://pubmed.ncbi.nlm.nih.gov/39378879
15. Wikipedia. Holobiont. Accessed 20 January 2025.
https://en.wikipedia.org/wiki/Holobiont
16. Magnúsdóttir S, Ravcheev D, de Crécy-Lagard V, Thiele I. Systematic genome assessment of B-vitamin biosynthesis suggests co-operation among gut microbes. Front Genet. 2015 Apr 20;6:148. doi: 10.3389/fgene.2015.00148. PMID: 25941533; PMCID: PMC4403557.
https://pubmed.ncbi.nlm.nih.gov/25941533
Microbiota and appetite
17. Fetissov SO. Role of the gut microbiota in host appetite control: bacterial growth to animal feeding behaviour. Nat Rev Endocrinol. 2017 Jan;13(1):11-25. doi: 10.1038/nrendo.2016.150. Epub 2016 Sep 12. PMID: 27616451.
https://pubmed.ncbi.nlm.nih.gov/27616451
17a. Roura E, Foster SR. Nutrient-Sensing Biology in Mammals and Birds. Annu Rev Anim Biosci. 2018 Feb 15;6:197-225. doi: 10.1146/annurev-animal-030117-014740. Epub 2017 Nov 20. PMID: 29166126.
https://pubmed.ncbi.nlm.nih.gov/29166126
18. van de Wouw M, Schellekens H, Dinan TG, Cryan JF. Microbiota-Gut-Brain Axis: Modulator of Host Metabolism and Appetite. J Nutr. 2017 May;147(5):727-745. doi: 10.3945/jn.116.240481. Epub 2017 Mar 29. PMID: 28356427.
https://pubmed.ncbi.nlm.nih.gov/28356427
Sensing in the gut
19. Avetisyan M, Schill EM, Heuckeroth RO. Building a second brain in the bowel. J Clin Invest. 2015 Mar 2;125(3):899-907. doi: 10.1172/JCI76307. Epub 2015 Feb 9. PMID: 25664848; PMCID: PMC4362233.
https://pubmed.ncbi.nlm.nih.gov/25664848
20. Janssen S, Depoortere I. Nutrient sensing in the gut: new roads to therapeutics? Trends Endocrinol Metab. 2013 Feb;24(2):92-100. doi: 10.1016/j.tem.2012.11.006. Epub 2012 Dec 21. PMID: 23266105.
https://pubmed.ncbi.nlm.nih.gov/23266105
21. Stanley S, Wynne K, McGowan B, Bloom S. Hormonal regulation of food intake. Physiol Rev. 2005 Oct;85(4):1131-58. doi: 10.1152/physrev.00015.2004. PMID: 16183909.
https://pubmed.ncbi.nlm.nih.gov/16183909
22. Spreckley E, Murphy KG. The L-Cell in Nutritional Sensing and the Regulation of Appetite. Front Nutr. 2015 Jul 20;2:23. doi: 10.3389/fnut.2015.00023. PMID: 26258126; PMCID: PMC4507148.
https://pubmed.ncbi.nlm.nih.gov/26258126
23. Wellendorph P, Johansen LD, Bräuner-Osborne H. Molecular pharmacology of promiscuous seven transmembrane receptors sensing organic nutrients. Mol Pharmacol. 2009 Sep;76(3):453-65. doi: 10.1124/mol.109.055244. Epub 2009 Jun 1. PMID: 19487246.
https://pubmed.ncbi.nlm.nih.gov/19487246
24. Blad CC, Tang C, Offermanns S. G protein-coupled receptors for energy metabolites as new therapeutic targets. Nat Rev Drug Discov. 2012 Aug;11(8):603-19. doi: 10.1038/nrd3777. Epub 2012 Jul 13. PMID: 22790105.
https://pubmed.ncbi.nlm.nih.gov/22790105
25. Woods SC. Gastrointestinal satiety signals I. An overview of gastrointestinal signals that influence food intake. Am J Physiol Gastrointest Liver Physiol. 2004 Jan;286(1):G7-13. doi: 10.1152/ajpgi.00448.2003. PMID: 14665437.
https://pubmed.ncbi.nlm.nih.gov/14665437
26. Murphy KG, Bloom SR. Gut hormones and the regulation of energy homeostasis. Nature. 2006 Dec 14;444(7121):854-9. doi: 10.1038/nature05484. PMID: 17167473.
https://pubmed.ncbi.nlm.nih.gov/17167473
27. Drucker DJ. The role of gut hormones in glucose homeostasis. J Clin Invest. 2007 Jan;117(1):24-32. doi: 10.1172/JCI30076. PMID: 17200703; PMCID: PMC1716213.
https://pubmed.ncbi.nlm.nih.gov/17200703
28. Dockray GJ. Gastrointestinal hormones and the dialogue between gut and brain. J Physiol. 2014 Jul 15;592(14):2927-41. doi: 10.1113/jphysiol.2014.270850. Epub 2014 Feb 24. PMID: 24566540; PMCID: PMC4214649.
https://pubmed.ncbi.nlm.nih.gov/24566540
29. Cryan JF, O’Mahony SM. The microbiome-gut-brain axis: from bowel to behavior. Neurogastroenterol Motil. 2011 Mar;23(3):187-92. doi: 10.1111/j.1365-2982.2010.01664.x. PMID: 21303428.
https://pubmed.ncbi.nlm.nih.gov/21303428
30. Bienenstock J, Collins S. 99th Dahlem conference on infection, inflammation and chronic inflammatory disorders: psycho-neuroimmunology and the intestinal microbiota: clinical observations and basic mechanisms. Clin Exp Immunol. 2010 Apr;160(1):85-91. doi: 10.1111/j.1365-2249.2010.04124.x. PMID: 20415856; PMCID: PMC2841840.
https://pubmed.ncbi.nlm.nih.gov/20415856
31. Dinan TG, Cryan JF. The Microbiome-Gut-Brain Axis in Health and Disease. Gastroenterol Clin North Am. 2017 Mar;46(1):77-89. doi: 10.1016/j.gtc.2016.09.007. Epub 2017 Jan 4. PMID: 28164854.
https://pubmed.ncbi.nlm.nih.gov/28164854
32. Montiel-Castro AJ, González-Cervantes RM, Bravo-Ruiseco G, Pacheco-López G. The microbiota-gut-brain axis: neurobehavioral correlates, health and sociality. Front Integr Neurosci. 2013 Oct 7;7:70. doi: 10.3389/fnint.2013.00070. PMID: 24109440; PMCID: PMC3791857.
https://pubmed.ncbi.nlm.nih.gov/24109440
33. Smith PA. The tantalizing links between gut microbes and the brain. Nature. 2015 Oct 15;526(7573):312-4. doi: 10.1038/526312a. PMID: 26469024.
https://pubmed.ncbi.nlm.nih.gov/26469024
34. Foster JA, McVey Neufeld KA. Gut-brain axis: how the microbiome influences anxiety and depression. Trends Neurosci. 2013 May;36(5):305-12. doi: 10.1016/j.tins.2013.01.005. Epub 2013 Feb 4. PMID: 23384445.
https://pubmed.ncbi.nlm.nih.gov/23384445
35. Schmidt C. Mental health: thinking from the gut. Nature. 2015 Feb 26;518(7540):S12-5. doi: 10.1038/518S13a. PMID: 25715275.
https://pubmed.ncbi.nlm.nih.gov/25715275
36. Sinagra E, Utzeri E, Morreale GC, Fabbri C, Pace F, Anderloni A. Microbiota-gut-brain axis and its affect inflammatory bowel disease: Pathophysiological concepts and insights for clinicians. World J Clin Cases. 2020 Mar 26;8(6):1013-1025. doi: 10.12998/wjcc.v8.i6.1013. PMID: 32258072; PMCID: PMC7103973.
https://pubmed.ncbi.nlm.nih.gov/32258072
37. Sarkar A, Lehto SM, Harty S, Dinan TG, Cryan JF, Burnet PWJ. Psychobiotics and the Manipulation of Bacteria-Gut-Brain Signals. Trends Neurosci. 2016 Nov;39(11):763-781. doi: 10.1016/j.tins.2016.09.002. Epub 2016 Oct 25. PMID: 27793434; PMCID: PMC5102282.
https://pubmed.ncbi.nlm.nih.gov/27793434
38. Gawałko M, Agbaedeng TA, Saljic A, Müller DN, Wilck N, Schnabel R, Penders J, Rienstra M, van Gelder I, Jespersen T, Schotten U, Crijns HJGM, Kalman JM, Sanders P, Nattel S, Dobrev D, Linz D. Gut microbiota, dysbiosis and atrial fibrillation. Arrhythmogenic mechanisms and potential clinical implications. Cardiovasc Res. 2022 Aug 24;118(11):2415-2427. doi: 10.1093/cvr/cvab292. PMID: 34550344; PMCID: PMC9400433.
https://pubmed.ncbi.nlm.nih.gov/34550344
39. Sinagra E, Utzeri E, Morreale GC, Fabbri C, Pace F, Anderloni A. Microbiota-gut-brain axis and its affect inflammatory bowel disease: Pathophysiological concepts and insights for clinicians. World J Clin Cases. 2020 Mar 26;8(6):1013-1025. doi: 10.12998/wjcc.v8.i6.1013. PMID: 32258072; PMCID: PMC7103973.
https://pubmed.ncbi.nlm.nih.gov/32258072
40. Carabotti M, Scirocco A, Maselli MA, Severi C. The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Ann Gastroenterol. 2015 Apr-Jun;28(2):203-209. PMID: 25830558; PMCID: PMC4367209.
https://pubmed.ncbi.nlm.nih.gov/25830558
41. Moens E, Veldhoen M. Epithelial barrier biology: good fences make good neighbours. Immunology. 2012 Jan;135(1):1-8. doi: 10.1111/j.1365-2567.2011.03506.x. PMID: 22044254; PMCID: PMC3246647.
https://pubmed.ncbi.nlm.nih.gov/22044254
42. Cryan JF, Dinan TG. Mind-altering microorganisms: the impact of the gut microbiota on brain and behaviour. Nat Rev Neurosci. 2012 Oct;13(10):701-12. doi: 10.1038/nrn3346. Epub 2012 Sep 12. PMID: 22968153.
https://pubmed.ncbi.nlm.nih.gov/22968153
43. Diet, Gut Microbiota and Obesity, L., Siniscalco, D., Bravaccio, C., & Loguercio, C. (2016). Gut–Brain Axis: A New Revolution to Understand the Pathogenesis of Autism and Other Severe Neurological Diseases. Human Nutrition from the Gastroenterologist’s Perspective: Lessons from Expo Milano 2015, 49-65.
https://link.springer.com/chapter/10.1007/978-3-319-30361-1_4
44. Bienenstock J, Collins S. 99th Dahlem conference on infection, inflammation and chronic inflammatory disorders: psycho-neuroimmunology and the intestinal microbiota: clinical observations and basic mechanisms. Clin Exp Immunol. 2010 Apr;160(1):85-91. doi: 10.1111/j.1365-2249.2010.04124.x. PMID: 20415856; PMCID: PMC2841840.
https://pubmed.ncbi.nlm.nih.gov/20415856
45. Montiel-Castro AJ, González-Cervantes RM, Bravo-Ruiseco G, Pacheco-López G. The microbiota-gut-brain axis: neurobehavioral correlates, health and sociality. Front Integr Neurosci. 2013 Oct 7;7:70. doi: 10.3389/fnint.2013.00070. PMID: 24109440; PMCID: PMC3791857.
https://pubmed.ncbi.nlm.nih.gov/24109440
46. Muskiet MHA, Wheeler DC, Heerspink HJL. New pharmacological strategies for protecting kidney function in type 2 diabetes. Lancet Diabetes Endocrinol. 2019 May;7(5):397-412. doi: 10.1016/S2213-8587(18)30263-8. Epub 2018 Dec 19. Erratum in: Lancet Diabetes Endocrinol. 2019 May;7(5):e5. doi: 10.1016/S2213-8587(19)30035-X. PMID: 30579729.
https://pubmed.ncbi.nlm.nih.gov/30579729
47. Nicholson JK, Holmes E, Kinross J, Burcelin R, Gibson G, Jia W, Pettersson S. Host-gut microbiota metabolic interactions. Science. 2012 Jun 8;336(6086):1262-7. doi: 10.1126/science.1223813. Epub 2012 Jun 6. PMID: 22674330.
https://pubmed.ncbi.nlm.nih.gov/22674330
48. Kashtanova DA, Popenko AS, Tkacheva ON, Tyakht AB, Alexeev DG, Boytsov SA. Association between the gut microbiota and diet: Fetal life, early childhood, and further life. Nutrition. 2016 Jun;32(6):620-7. doi: 10.1016/j.nut.2015.12.037. Epub 2015 Dec 31. PMID: 26946974.
https://pubmed.ncbi.nlm.nih.gov/26946974
49. Sharon G, Garg N, Debelius J, Knight R, Dorrestein PC, Mazmanian SK. Specialized metabolites from the microbiome in health and disease. Cell Metab. 2014 Nov 4;20(5):719-730. doi: 10.1016/j.cmet.2014.10.016. Epub 2014 Nov 4. PMID: 25440054; PMCID: PMC4337795.
https://pubmed.ncbi.nlm.nih.gov/25440054
50. Holmes E, Li JV, Marchesi JR, Nicholson JK. Gut microbiota composition and activity in relation to host metabolic phenotype and disease risk. Cell Metab. 2012 Nov 7;16(5):559-64. doi: 10.1016/j.cmet.2012.10.007. PMID: 23140640.
https://pubmed.ncbi.nlm.nih.gov/23140640
51. Petersen C. D-lactic acidosis. Nutr Clin Pract. 2005 Dec;20(6):634-45. doi: 10.1177/0115426505020006634. PMID: 16306301.
https://pubmed.ncbi.nlm.nih.gov/16306301
52. Lord RS, Bralley JA. Clinical applications of urinary organic acids. Part 2. Dysbiosis markers. Altern Med Rev. 2008 Dec;13(4):292-306. PMID: 19152477.
https://pubmed.ncbi.nlm.nih.gov/19152477
53. Galland L. The gut microbiome and the brain. J Med Food. 2014 Dec;17(12):1261-72. doi: 10.1089/jmf.2014.7000. PMID: 25402818; PMCID: PMC4259177.
https://pubmed.ncbi.nlm.nih.gov/25402818
54. Louis P, Scott KP, Duncan SH, Flint HJ. Understanding the effects of diet on bacterial metabolism in the large intestine. J Appl Microbiol. 2007 May;102(5):1197-208. doi: 10.1111/j.1365-2672.2007.03322.x. PMID: 17448155.
https://pubmed.ncbi.nlm.nih.gov/17448155
55. Degnan PH, Barry NA, Mok KC, Taga ME, Goodman AL. Human gut microbes use multiple transporters to distinguish vitamin B₁₂ analogs and compete in the gut. Cell Host Microbe. 2014 Jan 15;15(1):47-57. doi: 10.1016/j.chom.2013.12.007. PMID: 24439897; PMCID: PMC3923405.
https://pubmed.ncbi.nlm.nih.gov/24439897
56. Degnan PH, Barry NA, Mok KC, Taga ME, Goodman AL. Human gut microbes use multiple transporters to distinguish vitamin B₁₂ analogs and compete in the gut. Cell Host Microbe. 2014 Jan 15;15(1):47-57. doi: 10.1016/j.chom.2013.12.007. PMID: 24439897; PMCID: PMC3923405.
https://pubmed.ncbi.nlm.nih.gov/24439897
57. Baumgartner MR, Hörster F, Dionisi-Vici C, Haliloglu G, Karall D, Chapman KA, Huemer M, Hochuli M, Assoun M, Ballhausen D, Burlina A, Fowler B, Grünert SC, Grünewald S, Honzik T, Merinero B, Pérez-Cerdá C, Scholl-Bürgi S, Skovby F, Wijburg F, MacDonald A, Martinelli D, Sass JO, Valayannopoulos V, Chakrapani A. Proposed guidelines for the diagnosis and management of methylmalonic and propionic acidemia. Orphanet J Rare Dis. 2014 Sep 2;9:130. doi: 10.1186/s13023-014-0130-8. PMID: 25205257; PMCID: PMC4180313.
https://pubmed.ncbi.nlm.nih.gov/25205257
58. Sentongo TA, Azzam R, Charrow J. Vitamin B12 status, methylmalonic acidemia, and bacterial overgrowth in short bowel syndrome. J Pediatr Gastroenterol Nutr. 2009 Apr;48(4):495-7. doi: 10.1097/MPG.0b013e31817f9e5b. PMID: 19322060.
https://pubmed.ncbi.nlm.nih.gov/19322060
59. Macfabe DF. Short-chain fatty acid fermentation products of the gut microbiome: implications in autism spectrum disorders. Microb Ecol Health Dis. 2012 Aug 24;23. doi: 10.3402/mehd.v23i0.19260. PMID: 23990817; PMCID: PMC3747729.
https://pubmed.ncbi.nlm.nih.gov/23990817
60. Toh MC, Allen-Vercoe E. The human gut microbiota with reference to autism spectrum disorder: considering the whole as more than a sum of its parts. Microb Ecol Health Dis. 2015 Jan 28;26:26309. doi: 10.3402/mehd.v26.26309. PMID: 25634609; PMCID: PMC4310852.
https://pubmed.ncbi.nlm.nih.gov/25634609
61. Finegold SM, Dowd SE, Gontcharova V, Liu C, Henley KE, Wolcott RD, Youn E, Summanen PH, Granpeesheh D, Dixon D, Liu M, Molitoris DR, Green JA 3rd. Pyrosequencing study of fecal microflora of autistic and control children. Anaerobe. 2010 Aug;16(4):444-53. doi: 10.1016/j.anaerobe.2010.06.008. Epub 2010 Jul 9. PMID: 20603222.
https://pubmed.ncbi.nlm.nih.gov/20603222
62. Morath MA, Okun JG, Müller IB, Sauer SW, Hörster F, Hoffmann GF, Kölker S. Neurodegeneration and chronic renal failure in methylmalonic aciduria–a pathophysiological approach. J Inherit Metab Dis. 2008 Feb;31(1):35-43. doi: 10.1007/s10545-007-0571-5. Epub 2007 Sep 12. PMID: 17846917.
https://pubmed.ncbi.nlm.nih.gov/17846917
63. Green R. Cobalamin supplements for infants: a shot in the cradle? Am J Clin Nutr. 2013 Nov;98(5):1149-50. doi: 10.3945/ajcn.113.074054. Epub 2013 Sep 25. PMID: 24067668.
https://pubmed.ncbi.nlm.nih.gov/24067668
64. Koeth RA, Wang Z, Levison BS, Buffa JA, Org E, Sheehy BT, Britt EB, Fu X, Wu Y, Li L, Smith JD, DiDonato JA, Chen J, Li H, Wu GD, Lewis JD, Warrier M, Brown JM, Krauss RM, Tang WH, Bushman FD, Lusis AJ, Hazen SL. Intestinal microbiota metabolism of L-carnitine, a nutrient in red meat, promotes atherosclerosis. Nat Med. 2013 May;19(5):576-85. doi: 10.1038/nm.3145. Epub 2013 Apr 7. PMID: 23563705; PMCID: PMC3650111.
https://pubmed.ncbi.nlm.nih.gov/23563705
65. Wang Z, Klipfell E, Bennett BJ, Koeth R, Levison BS, Dugar B, Feldstein AE, Britt EB, Fu X, Chung YM, Wu Y, Schauer P, Smith JD, Allayee H, Tang WH, DiDonato JA, Lusis AJ, Hazen SL. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature. 2011 Apr 7;472(7341):57-63. doi: 10.1038/nature09922. PMID: 21475195; PMCID: PMC3086762.
https://pubmed.ncbi.nlm.nih.gov/21475195
66. Tang WH, Wang Z, Levison BS, Koeth RA, Britt EB, Fu X, Wu Y, Hazen SL. Intestinal microbial metabolism of phosphatidylcholine and cardiovascular risk. N Engl J Med. 2013 Apr 25;368(17):1575-84. doi: 10.1056/NEJMoa1109400. PMID: 23614584; PMCID: PMC3701945.
https://pubmed.ncbi.nlm.nih.gov/23614584
67. Round JL, Mazmanian SK. The gut microbiota shapes intestinal immune responses during health and disease. Nat Rev Immunol. 2009 May;9(5):313-23. doi: 10.1038/nri2515. Erratum in: Nat Rev Immunol. 2009 Aug;9(8):600. PMID: 19343057; PMCID: PMC4095778.
https://pubmed.ncbi.nlm.nih.gov/19343057
68. Tuohy KM, Fava F, Viola R. ‘The way to a man’s heart is through his gut microbiota’–dietary pro- and prebiotics for the management of cardiovascular risk. Proc Nutr Soc. 2014 May;73(2):172-85. doi: 10.1017/S0029665113003911. Epub 2014 Feb 4. PMID: 24495527.
https://pubmed.ncbi.nlm.nih.gov/24495527
69. Kim E, Coelho D, Blachier F. Review of the association between meat consumption and risk of colorectal cancer. Nutr Res. 2013 Dec;33(12):983-94. doi: 10.1016/j.nutres.2013.07.018. Epub 2013 Oct 7. PMID: 24267037.
https://pubmed.ncbi.nlm.nih.gov/24267037
70. Lord RS, Bralley JA. Clinical applications of urinary organic acids. Part 2. Dysbiosis markers. Altern Med Rev. 2008 Dec;13(4):292-306. PMID: 19152477.
https://pubmed.ncbi.nlm.nih.gov/19152477
71. Sekirov I, Russell SL, Antunes LC, Finlay BB. Gut microbiota in health and disease. Physiol Rev. 2010 Jul;90(3):859-904. doi: 10.1152/physrev.00045.2009. PMID: 20664075.
https://pubmed.ncbi.nlm.nih.gov/20664075
73. Cani PD, Delzenne NM. The role of the gut microbiota in energy metabolism and metabolic disease. Curr Pharm Des. 2009;15(13):1546-58. doi: 10.2174/138161209788168164. PMID: 19442172.
https://pubmed.ncbi.nlm.nih.gov/19442172
74. Johnson AM, Olefsky JM. The origins and drivers of insulin resistance. Cell. 2013 Feb 14;152(4):673-84. doi: 10.1016/j.cell.2013.01.041. PMID: 23415219.
https://pubmed.ncbi.nlm.nih.gov/23415219
75. Diamant M, Blaak EE, de Vos WM. Do nutrient-gut-microbiota interactions play a role in human obesity, insulin resistance and type 2 diabetes? Obes Rev. 2011 Apr;12(4):272-81. doi: 10.1111/j.1467-789X.2010.00797.x. Epub 2010 Aug 26. PMID: 20804522.
https://pubmed.ncbi.nlm.nih.gov/20804522
76. Nakamura YK, Omaye ST. Metabolic diseases and pro- and prebiotics: Mechanistic insights. Nutr Metab (Lond). 2012 Jun 19;9(1):60. doi: 10.1186/1743-7075-9-60. PMID: 22713169; PMCID: PMC3464869.
https://pubmed.ncbi.nlm.nih.gov/22713169
77. Gérard P. Gut microbiota and obesity. Cell Mol Life Sci. 2016 Jan;73(1):147-62. doi: 10.1007/s00018-015-2061-5. Epub 2015 Oct 12. PMID: 26459447; PMCID: PMC11108539.
https://pubmed.ncbi.nlm.nih.gov/26459447
78. Liu BN, Liu XT, Liang ZH, Wang JH. Gut microbiota in obesity. World J Gastroenterol. 2021 Jul 7;27(25):3837-3850. doi: 10.3748/wjg.v27.i25.3837. PMID: 34321848; PMCID: PMC8291023.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8291023/#sec14
79. Li, H., & Wei, C. (2015). Diet, gut microbiota and obesity. J. Nutr. Health Food Sci, 3, 1-6.
https://hongjielilab.org/wp-content/uploads/2020/10/2015-li-jnhfs.pdf
80. Das UN. Obesity: genes, brain, gut, and environment. Nutrition. 2010 May;26(5):459-73. doi: 10.1016/j.nut.2009.09.020. Epub 2009 Dec 22. PMID: 20022465.
https://pubmed.ncbi.nlm.nih.gov/20022465
81. Hartstra AV, Bouter KE, Bäckhed F, Nieuwdorp M. Insights into the role of the microbiome in obesity and type 2 diabetes. Diabetes Care. 2015 Jan;38(1):159-65. doi: 10.2337/dc14-0769. PMID: 25538312.
https://pubmed.ncbi.nlm.nih.gov/25538312
82. Caricilli AM, Saad MJ. The role of gut microbiota on insulin resistance. Nutrients. 2013 Mar 12;5(3):829-51. doi: 10.3390/nu5030829. PMID: 23482058; PMCID: PMC3705322.
https://pubmed.ncbi.nlm.nih.gov/23482058
83. Ley RE, Turnbaugh PJ, Klein S, Gordon JI. Microbial ecology: human gut microbes associated with obesity. Nature. 2006 Dec 21;444(7122):1022-3. doi: 10.1038/4441022a. PMID: 17183309.
https://pubmed.ncbi.nlm.nih.gov/17183309
84. Patterson E, Ryan PM, Cryan JF, Dinan TG, Ross RP, Fitzgerald GF, Stanton C. Gut microbiota, obesity and diabetes. Postgrad Med J. 2016 May;92(1087):286-300. doi: 10.1136/postgradmedj-2015-133285. Epub 2016 Feb 24. PMID: 26912499.
https://pubmed.ncbi.nlm.nih.gov/26912499
85. Koliada A, Syzenko G, Moseiko V, Budovska L, Puchkov K, Perederiy V, Gavalko Y, Dorofeyev A, Romanenko M, Tkach S, Sineok L, Lushchak O, Vaiserman A. Association between body mass index and Firmicutes/Bacteroidetes ratio in an adult Ukrainian population. BMC Microbiol. 2017 May 22;17(1):120. doi: 10.1186/s12866-017-1027-1. PMID: 28532414; PMCID: PMC5440985.
https://pubmed.ncbi.nlm.nih.gov/28532414
86. Caricilli AM, Saad MJ. Gut microbiota composition and its effects on obesity and insulin resistance. Curr Opin Clin Nutr Metab Care. 2014 Jul;17(4):312-8. doi: 10.1097/MCO.0000000000000067. PMID: 24848531.
https://pubmed.ncbi.nlm.nih.gov/24848531
87. Caricilli AM, Saad MJ. Gut microbiota composition and its effects on obesity and insulin resistance. Curr Opin Clin Nutr Metab Care. 2014 Jul;17(4):312-8. doi: 10.1097/MCO.0000000000000067. PMID: 24848531.
https://pubmed.ncbi.nlm.nih.gov/24848531
88. Krajmalnik-Brown R, Ilhan ZE, Kang DW, DiBaise JK. Effects of gut microbes on nutrient absorption and energy regulation. Nutr Clin Pract. 2012 Apr;27(2):201-14. doi: 10.1177/0884533611436116. Epub 2012 Feb 24. PMID: 22367888; PMCID: PMC3601187.
https://pubmed.ncbi.nlm.nih.gov/22367888
89. Henningsson AM, Björck IM, Nyman EM. Combinations of indigestible carbohydrates affect short-chain fatty acid formation in the hindgut of rats. J Nutr. 2002 Oct;132(10):3098-104. doi: 10.1093/jn/131.10.3098. PMID: 12368401.
https://pubmed.ncbi.nlm.nih.gov/12368401
90. Wong JM, de Souza R, Kendall CW, Emam A, Jenkins DJ. Colonic health: fermentation and short chain fatty acids. J Clin Gastroenterol. 2006 Mar;40(3):235-43. doi: 10.1097/00004836-200603000-00015. PMID: 16633129.
https://pubmed.ncbi.nlm.nih.gov/16633129
91. Kimura I, Ozawa K, Inoue D, Imamura T, Kimura K, Maeda T, Terasawa K, Kashihara D, Hirano K, Tani T, Takahashi T, Miyauchi S, Shioi G, Inoue H, Tsujimoto G. The gut microbiota suppresses insulin-mediated fat accumulation via the short-chain fatty acid receptor GPR43. Nat Commun. 2013;4:1829. doi: 10.1038/ncomms2852. PMID: 23652017; PMCID: PMC3674247.
https://pubmed.ncbi.nlm.nih.gov/23652017
92. Macia L, Thorburn AN, Binge LC, Marino E, Rogers KE, Maslowski KM, Vieira AT, Kranich J, Mackay CR. Microbial influences on epithelial integrity and immune function as a basis for inflammatory diseases. Immunol Rev. 2012 Jan;245(1):164-76. doi: 10.1111/j.1600-065X.2011.01080.x. PMID: 22168419.
https://pubmed.ncbi.nlm.nih.gov/22168419
93. Louis P, Scott KP, Duncan SH, Flint HJ. Understanding the effects of diet on bacterial metabolism in the large intestine. J Appl Microbiol. 2007 May;102(5):1197-208. doi: 10.1111/j.1365-2672.2007.03322.x. PMID: 17448155.
https://pubmed.ncbi.nlm.nih.gov/17448155
94. Pryde SE, Duncan SH, Hold GL, Stewart CS, Flint HJ. The microbiology of butyrate formation in the human colon. FEMS Microbiol Lett. 2002 Dec 17;217(2):133-9. doi: 10.1111/j.1574-6968.2002.tb11467.x. PMID: 12480096.
https://pubmed.ncbi.nlm.nih.gov/12480096
95. Scott KP, Antoine JM, Midtvedt T, van Hemert S. Manipulating the gut microbiota to maintain health and treat disease. Microb Ecol Health Dis. 2015 Feb 2;26:25877. doi: 10.3402/mehd.v26.25877. PMID: 25651995; PMCID: PMC4315778.
https://pubmed.ncbi.nlm.nih.gov/25651995
96. Plöger S, Stumpff F, Penner GB, Schulzke JD, Gäbel G, Martens H, Shen Z, Günzel D, Aschenbach JR. Microbial butyrate and its role for barrier function in the gastrointestinal tract. Ann N Y Acad Sci. 2012 Jul;1258:52-9. doi: 10.1111/j.1749-6632.2012.06553.x. PMID: 22731715.
https://pubmed.ncbi.nlm.nih.gov/22731715
97. Belcheva A, Irrazabal T, Martin A. Gut microbial metabolism and colon cancer: can manipulations of the microbiota be useful in the management of gastrointestinal health? Bioessays. 2015 Apr;37(4):403-12. doi: 10.1002/bies.201400204. Epub 2015 Jan 20. PMID: 25601287.
https://pubmed.ncbi.nlm.nih.gov/25601287
98. Jumpertz R, Le DS, Turnbaugh PJ, Trinidad C, Bogardus C, Gordon JI, Krakoff J. Energy-balance studies reveal associations between gut microbes, caloric load, and nutrient absorption in humans. Am J Clin Nutr. 2011 Jul;94(1):58-65. doi: 10.3945/ajcn.110.010132. Epub 2011 May 4. PMID: 21543530; PMCID: PMC3127503.
https://pubmed.ncbi.nlm.nih.gov/21543530
99. Caricilli AM, Saad MJ. Gut microbiota composition and its effects on obesity and insulin resistance. Curr Opin Clin Nutr Metab Care. 2014 Jul;17(4):312-8. doi: 10.1097/MCO.0000000000000067. PMID: 24848531.
https://pubmed.ncbi.nlm.nih.gov/24848531
100. O’Connor EM, O’Herlihy EA, O’Toole PW. Gut microbiota in older subjects: variation, health consequences and dietary intervention prospects. Proc Nutr Soc. 2014 Nov;73(4):441-51. doi: 10.1017/S0029665114000597. Epub 2014 May 13. PMID: 24824449.
https://pubmed.ncbi.nlm.nih.gov/24824449
101. Raetz CR, Reynolds CM, Trent MS, Bishop RE. Lipid A modification systems in gram-negative bacteria. Annu Rev Biochem. 2007;76:295-329. doi: 10.1146/annurev.biochem.76.010307.145803. PMID: 17362200; PMCID: PMC2569861.
https://pubmed.ncbi.nlm.nih.gov/17362200
102. Bengmark S. Gut microbiota, immune development and function. Pharmacol Res. 2013 Mar;69(1):87-113. doi: 10.1016/j.phrs.2012.09.002. Epub 2012 Sep 16. PMID: 22989504.
https://pubmed.ncbi.nlm.nih.gov/22989504
103. Caricilli AM, Saad MJ. The role of gut microbiota on insulin resistance. Nutrients. 2013 Mar 12;5(3):829-51. doi: 10.3390/nu5030829. PMID: 23482058; PMCID: PMC3705322.
https://pubmed.ncbi.nlm.nih.gov/23482058
104. Caesar R, Fåk F, Bäckhed F. Effects of gut microbiota on obesity and atherosclerosis via modulation of inflammation and lipid metabolism. J Intern Med. 2010 Oct;268(4):320-8. doi: 10.1111/j.1365-2796.2010.02270.x. PMID: 21050286.
https://pubmed.ncbi.nlm.nih.gov/21050286
105. Land WG. Chronic allograft dysfunction: a model disorder of innate immunity. Biomed J. 2013 Sep-Oct;36(5):209-28. doi: 10.4103/2319-4170.117622. PMID: 24225188.
https://pubmed.ncbi.nlm.nih.gov/24225188
106. Erridge C. Diet, commensals and the intestine as sources of pathogen-associated molecular patterns in atherosclerosis, type 2 diabetes and non-alcoholic fatty liver disease. Atherosclerosis. 2011 May;216(1):1-6. doi: 10.1016/j.atherosclerosis.2011.02.043. Epub 2011 Feb 26. PMID: 21439567.
https://pubmed.ncbi.nlm.nih.gov/21439567
107. Margioris AN. Fatty acids and postprandial inflammation. Curr Opin Clin Nutr Metab Care. 2009 Mar;12(2):129-37. doi: 10.1097/MCO.0b013e3283232a11. PMID: 19202384.
https://pubmed.ncbi.nlm.nih.gov/19202384
108. Moreira AP, Texeira TF, Ferreira AB, Peluzio Mdo C, Alfenas Rde C. Influence of a high-fat diet on gut microbiota, intestinal permeability and metabolic endotoxaemia. Br J Nutr. 2012 Sep;108(5):801-9. doi: 10.1017/S0007114512001213. Epub 2012 Apr 16. PMID: 22717075.
https://pubmed.ncbi.nlm.nih.gov/22717075
109. Neuschwander-Tetri BA. Carbohydrate intake and nonalcoholic fatty liver disease. Curr Opin Clin Nutr Metab Care. 2013 Jul;16(4):446-52. doi: 10.1097/MCO.0b013e328361c4d1. PMID: 23657151.
https://pubmed.ncbi.nlm.nih.gov/23657151
110. Carvalho BM, Saad MJ. Influence of gut microbiota on subclinical inflammation and insulin resistance. Mediators Inflamm. 2013;2013:986734. doi: 10.1155/2013/986734. Epub 2013 Jun 12. PMID: 23840101; PMCID: PMC3694527..
https://pubmed.ncbi.nlm.nih.gov/23840101
111. Tsukumo DM, Carvalho BM, Carvalho Filho MA, Saad MJ. Translational research into gut microbiota: new horizons on obesity treatment: updated 2014. Arch Endocrinol Metab. 2015 Apr;59(2):154-60. doi: 10.1590/2359-3997000000029. Epub 2015 Apr 1. PMID: 25993679.
https://pubmed.ncbi.nlm.nih.gov/25993679
112. Vrieze A, Holleman F, Zoetendal EG, de Vos WM, Hoekstra JB, Nieuwdorp M. The environment within: how gut microbiota may influence metabolism and body composition. Diabetologia. 2010 Apr;53(4):606-13. doi: 10.1007/s00125-010-1662-7. Epub 2010 Jan 26. PMID: 20101384; PMCID: PMC2830587.
https://pubmed.ncbi.nlm.nih.gov/20101384
113. Parekh PJ, Arusi E, Vinik AI, Johnson DA. The role and influence of gut microbiota in pathogenesis and management of obesity and metabolic syndrome. Front Endocrinol (Lausanne). 2014 Apr 7;5:47. doi: 10.3389/fendo.2014.00047. PMID: 24778627; PMCID: PMC3984999.
https://pubmed.ncbi.nlm.nih.gov/24778627
114. de Vos WM, Nieuwdorp M. Genomics: A gut prediction. Nature. 2013 Jun 6;498(7452):48-9. doi: 10.1038/nature12251. Epub 2013 May 29. PMID: 23719383.
https://pubmed.ncbi.nlm.nih.gov/23719383
115. Karlsson FH, Tremaroli V, Nookaew I, Bergström G, Behre CJ, Fagerberg B, Nielsen J, Bäckhed F. Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature. 2013 Jun 6;498(7452):99-103. doi: 10.1038/nature12198. Epub 2013 May 29. PMID: 23719380.
https://pubmed.ncbi.nlm.nih.gov/23719380
116. Kelly JR, Minuto C, Cryan JF, Clarke G, Dinan TG. Cross Talk: The Microbiota and Neurodevelopmental Disorders. Front Neurosci. 2017 Sep 15;11:490. doi: 10.3389/fnins.2017.00490. PMID: 28966571; PMCID: PMC5605633.
https://pubmed.ncbi.nlm.nih.gov/28966571
117. Sherwin E, Dinan TG, Cryan JF. Recent developments in understanding the role of the gut microbiota in brain health and disease. Ann N Y Acad Sci. 2018 May;1420(1):5-25. doi: 10.1111/nyas.13416. Epub 2017 Aug 2. PMID: 28768369.
https://pubmed.ncbi.nlm.nih.gov/28768369
118. Mayer EA, Tillisch K, Gupta A. Gut/brain axis and the microbiota. J Clin Invest. 2015 Mar 2;125(3):926-38. doi: 10.1172/JCI76304. Epub 2015 Feb 17. PMID: 25689247; PMCID: PMC4362231.
https://pubmed.ncbi.nlm.nih.gov/25689247
119. Ghaisas S, Maher J, Kanthasamy A. Gut microbiome in health and disease: Linking the microbiome-gut-brain axis and environmental factors in the pathogenesis of systemic and neurodegenerative diseases. Pharmacol Ther. 2016 Feb;158:52-62. doi: 10.1016/j.pharmthera.2015.11.012. Epub 2015 Nov 26. PMID: 26627987; PMCID: PMC4747781.
https://pubmed.ncbi.nlm.nih.gov/26627987
120. Rogers GB, Keating DJ, Young RL, Wong ML, Licinio J, Wesselingh S. From gut dysbiosis to altered brain function and mental illness: mechanisms and pathways. Mol Psychiatry. 2016 Jun;21(6):738-48. doi: 10.1038/mp.2016.50. Epub 2016 Apr 19. PMID: 27090305; PMCID: PMC4879184.
https://pubmed.ncbi.nlm.nih.gov/27090305
121. Foster JA, Rinaman L, Cryan JF. Stress & the gut-brain axis: Regulation by the microbiome. Neurobiol Stress. 2017 Mar 19;7:124-136. doi: 10.1016/j.ynstr.2017.03.001. PMID: 29276734; PMCID: PMC5736941.
https://pubmed.ncbi.nlm.nih.gov/29276734
122. Vuong HE, Hsiao EY. Emerging Roles for the Gut Microbiome in Autism Spectrum Disorder. Biol Psychiatry. 2017 Mar 1;81(5):411-423. doi: 10.1016/j.biopsych.2016.08.024. Epub 2016 Aug 26. PMID: 27773355; PMCID: PMC5285286.
https://pubmed.ncbi.nlm.nih.gov/27773355
123. Li Q, Zhou JM. The microbiota-gut-brain axis and its potential therapeutic role in autism spectrum disorder. Neuroscience. 2016 Jun 2;324:131-9. doi: 10.1016/j.neuroscience.2016.03.013. Epub 2016 Mar 8. PMID: 26964681.
https://pubmed.ncbi.nlm.nih.gov/26964681
124. Alharthi A, Alhazmi S, Alburae N, Bahieldin A. The Human Gut Microbiome as a Potential Factor in Autism Spectrum Disorder. Int J Mol Sci. 2022 Jan 25;23(3):1363. doi: 10.3390/ijms23031363. PMID: 35163286; PMCID: PMC8835713.
https://pubmed.ncbi.nlm.nih.gov/35163286
125. Kelly JR, Borre Y, O’ Brien C, Patterson E, El Aidy S, Deane J, Kennedy PJ, Beers S, Scott K, Moloney G, Hoban AE, Scott L, Fitzgerald P, Ross P, Stanton C, Clarke G, Cryan JF, Dinan TG. Transferring the blues: Depression-associated gut microbiota induces neurobehavioural changes in the rat. J Psychiatr Res. 2016 Nov;82:109-18. doi: 10.1016/j.jpsychires.2016.07.019. Epub 2016 Jul 25. PMID: 27491067.
https://pubmed.ncbi.nlm.nih.gov/27491067
126. Schachter J, Martel J, Lin CS, Chang CJ, Wu TR, Lu CC, Ko YF, Lai HC, Ojcius DM, Young JD. Effects of obesity on depression: A role for inflammation and the gut microbiota. Brain Behav Immun. 2018 Mar;69:1-8. doi: 10.1016/j.bbi.2017.08.026. Epub 2017 Sep 6. PMID: 28888668.
https://pubmed.ncbi.nlm.nih.gov/28888668
127. Houser MC, Tansey MG. The gut-brain axis: is intestinal inflammation a silent driver of Parkinson’s disease pathogenesis? NPJ Parkinsons Dis. 2017 Jan 11;3:3. doi: 10.1038/s41531-016-0002-0. PMID: 28649603; PMCID: PMC5445611.
https://pubmed.ncbi.nlm.nih.gov/28649603
128. Grenham S, Clarke G, Cryan JF, Dinan TG. Brain-gut-microbe communication in health and disease. Front Physiol. 2011 Dec 7;2:94. doi: 10.3389/fphys.2011.00094. PMID: 22162969; PMCID: PMC3232439.
https://pubmed.ncbi.nlm.nih.gov/22162969
129. Kennedy PJ, Cryan JF, Dinan TG, Clarke G. Irritable bowel syndrome: a microbiome-gut-brain axis disorder? World J Gastroenterol. 2014 Oct 21;20(39):14105-25. doi: 10.3748/wjg.v20.i39.14105. PMID: 25339800; PMCID: PMC4202342.
https://pubmed.ncbi.nlm.nih.gov/25339800
130. O’Mahony SM, Clarke G, Borre YE, Dinan TG, Cryan JF. Serotonin, tryptophan metabolism and the brain-gut-microbiome axis. Behav Brain Res. 2015 Jan 15;277:32-48. doi: 10.1016/j.bbr.2014.07.027. Epub 2014 Jul 29. PMID: 25078296.
https://pubmed.ncbi.nlm.nih.gov/25078296
131. Fukuda K. Etiological classification of depression based on the enzymes of tryptophan metabolism. BMC Psychiatry. 2014 Dec 24;14:372. doi: 10.1186/s12888-014-0372-y. PMID: 25540092; PMCID: PMC4321701.
https://pubmed.ncbi.nlm.nih.gov/25540092
132. Kern L, Mastandrea I, Melekhova A, Elinav E. Mechanisms by which microbiome-derived metabolites exert their impacts on neurodegeneration. Cell Chem Biol. 2025 Jan 16;32(1):25-45. doi: 10.1016/j.chembiol.2024.08.014. Epub 2024 Sep 25. PMID: 39326420.
https://pubmed.ncbi.nlm.nih.gov/39326420
133. Welz L, Harris DM, Kim NM, Alsaadi AI, Wu Q, Oumari M, Taubenheim J, Volk V, Credido G, Koncina E, Mukherjee PK, Tran F, Sievers LK, Pavlidis P, Powell N, Rieder F, Letellier E, Waschina S, Kaleta C, Feuerhake F, Verstockt B, McReynolds MR, Rosenstiel P, Schreiber S, Aden K. A metabolic constraint in the kynurenine pathway drives mucosal inflammation in IBD. medRxiv [Preprint]. 2024 Aug 8:2024.08.08.24311598. doi: 10.1101/2024.08.08.24311598. PMID: 39211892; PMCID: PMC11361206.
https://pubmed.ncbi.nlm.nih.gov/39211892
134. Dewulf JP, Martin M, Marie S, Oguz F, Belkhir L, De Greef J, Yombi JC, Wittebole X, Laterre PF, Jadoul M, Gatto L, Bommer GT, Morelle J. Urine metabolomics links dysregulation of the tryptophan-kynurenine pathway to inflammation and severity of COVID-19. Sci Rep. 2022 Jun 15;12(1):9959. doi: 10.1038/s41598-022-14292-w. PMID: 35705608; PMCID: PMC9198612.
https://pubmed.ncbi.nlm.nih.gov/35705608
135. Gao K, Mu CL, Farzi A, Zhu WY. Tryptophan Metabolism: A Link Between the Gut Microbiota and Brain. Adv Nutr. 2020 May 1;11(3):709-723. doi: 10.1093/advances/nmz127. PMID: 31825083; PMCID: PMC7231603.
https://pubmed.ncbi.nlm.nih.gov/31825083
136. Kapoor B, Biswas P, Gulati M, Rani P, Gupta R. Gut microbiome and Alzheimer’s disease: What we know and what remains to be explored. Ageing Res Rev. 2024 Dec;102:102570. doi: 10.1016/j.arr.2024.102570. Epub 2024 Oct 30. PMID: 39486524.
https://pubmed.ncbi.nlm.nih.gov/39486524
137. Pan I, Issac PK, Rahman MM, Guru A, Arockiaraj J. Gut-Brain Axis a Key Player to Control Gut Dysbiosis in Neurological Diseases. Mol Neurobiol. 2024 Dec;61(12):9873-9891. doi: 10.1007/s12035-023-03691-3. Epub 2023 Oct 18. PMID: 37851313.
https://pubmed.ncbi.nlm.nih.gov/37851313
138. Kearns R. The Kynurenine Pathway in Gut Permeability and Inflammation. Inflammation. 2024 Sep 10. doi: 10.1007/s10753-024-02135-x. Epub ahead of print. PMID: 39256304.
https://pubmed.ncbi.nlm.nih.gov/39256304
139. Kearns R. Gut-Brain Axis and Neuroinflammation: The Role of Gut Permeability and the Kynurenine Pathway in Neurological Disorders. Cell Mol Neurobiol. 2024 Oct 8;44(1):64. doi: 10.1007/s10571-024-01496-z. PMID: 39377830; PMCID: PMC11461658.
https://pubmed.ncbi.nlm.nih.gov/39377830
140. Braidy N, Grant R. Kynurenine pathway metabolism and neuroinflammatory disease. Neural Regen Res. 2017 Jan;12(1):39-42. doi: 10.4103/1673-5374.198971. PMID: 28250737; PMCID: PMC5319230.
https://pubmed.ncbi.nlm.nih.gov/28250737
141. Wang H, Lee IS, Braun C, Enck P. Effect of Probiotics on Central Nervous System Functions in Animals and Humans: A Systematic Review. J Neurogastroenterol Motil. 2016 Oct 30;22(4):589-605. doi: 10.5056/jnm16018. PMID: 27413138; PMCID: PMC5056568.
https://pubmed.ncbi.nlm.nih.gov/27413138
Gut motility
142. Vahora IS, Tsouklidis N, Kumar R, Soni R, Khan S. How Serotonin Level Fluctuation Affects the Effectiveness of Treatment in Irritable Bowel Syndrome. Cureus. 2020 Aug 19;12(8):e9871. doi: 10.7759/cureus.9871. Erratum in: Cureus. 2020 Sep 1;12(9):c36. doi: 10.7759/cureus.c36. PMID: 32968548; PMCID: PMC7505258.
https://pmc.ncbi.nlm.nih.gov/articles/PMC7505258
143. Buey B, Forcén A, Grasa L, Layunta E, Mesonero JE, Latorre E. Gut Microbiota-Derived Short-Chain Fatty Acids: Novel Regulators of Intestinal Serotonin Transporter. Life (Basel). 2023 Apr 26;13(5):1085. doi: 10.3390/life13051085. PMID: 37240731; PMCID: PMC10221112.
https://pubmed.ncbi.nlm.nih.gov/37240731
144. Reigstad CS, Salmonson CE, Rainey JF 3rd, Szurszewski JH, Linden DR, Sonnenburg JL, Farrugia G, Kashyap PC. Gut microbes promote colonic serotonin production through an effect of short-chain fatty acids on enterochromaffin cells. FASEB J. 2015 Apr;29(4):1395-403. doi: 10.1096/fj.14-259598. Epub 2014 Dec 30. PMID: 25550456; PMCID: PMC4396604.
https://pubmed.ncbi.nlm.nih.gov/25550456
145. Yano JM, Yu K, Donaldson GP, Shastri GG, Ann P, Ma L, Nagler CR, Ismagilov RF, Mazmanian SK, Hsiao EY. Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell. 2015 Apr 9;161(2):264-76. doi: 10.1016/j.cell.2015.02.047. Erratum in: Cell. 2015 Sep 24;163:258. PMID: 25860609; PMCID: PMC4393509.
https://pmc.ncbi.nlm.nih.gov/articles/PMC4393509
Methane
146. Sahakian AB, Jee SR, Pimentel M. Methane and the gastrointestinal tract. Dig Dis Sci. 2010 Aug;55(8):2135-43. doi: 10.1007/s10620-009-1012-0. Epub 2009 Oct 15. PMID: 19830557.
https://pubmed.ncbi.nlm.nih.gov/19830557
147. Roccarina D, Lauritano EC, Gabrielli M, Franceschi F, Ojetti V, Gasbarrini A. The role of methane in intestinal diseases. Am J Gastroenterol. 2010 Jun;105(6):1250-6. doi: 10.1038/ajg.2009.744. Epub 2010 Mar 9. PMID: 20216536.
https://pubmed.ncbi.nlm.nih.gov/20216536
148. Kasarello K, Cudnoch-Jedrzejewska A, Czarzasta K. Communication of gut microbiota and brain via immune and neuroendocrine signaling. Front Microbiol. 2023 Jan 25;14:1118529. doi: 10.3389/fmicb.2023.1118529. PMID: 36760508; PMCID: PMC9907780.
https://pubmed.ncbi.nlm.nih.gov/36760508
149. van Donkelaar EL, Blokland A, Ferrington L, Kelly PA, Steinbusch HW, Prickaerts J. Mechanism of acute tryptophan depletion: is it only serotonin? Mol Psychiatry. 2011 Jul;16(7):695-713. doi: 10.1038/mp.2011.9. Epub 2011 Feb 22. PMID: 21339754.
https://pubmed.ncbi.nlm.nih.gov/21339754
Hunter Gatherers, diversity, eco-system, evolution
150. Rampelli S, Schnorr SL, Consolandi C, Turroni S, Severgnini M, Peano C, Brigidi P, Crittenden AN, Henry AG, Candela M. Metagenome Sequencing of the Hadza Hunter-Gatherer Gut Microbiota. Curr Biol. 2015 Jun 29;25(13):1682-93. doi: 10.1016/j.cub.2015.04.055. Epub 2015 May 14. PMID: 25981789.
https://pubmed.ncbi.nlm.nih.gov/25981789
150a. Clemente JC, Pehrsson EC, Blaser MJ, Sandhu K, Gao Z, Wang B, Magris M, Hidalgo G, Contreras M, Noya-Alarcón Ó, Lander O, McDonald J, Cox M, Walter J, Oh PL, Ruiz JF, Rodriguez S, Shen N, Song SJ, Metcalf J, Knight R, Dantas G, Dominguez-Bello MG. The microbiome of uncontacted Amerindians. Sci Adv. 2015 Apr 3;1(3):e1500183. doi: 10.1126/sciadv.1500183. PMID: 26229982; PMCID: PMC4517851.
https://pubmed.ncbi.nlm.nih.gov/26229982
150b. Abdill RJ, Graham SP, Rubinetti V, Ahmadian M, Hicks P, Chetty A, McDonald D, Ferretti P, Gibbons E, Rossi M, Krishnan A, Albert FW, Greene CS, Davis S, Blekhman R. Integration of 168,000 samples reveals global patterns of the human gut microbiome. Cell. 2025 Jan 16:S0092-8674(24)01430-2. doi: 10.1016/j.cell.2024.12.017. Epub ahead of print. PMID: 39848248.
https://pubmed.ncbi.nlm.nih.gov/39848248
150c. Chassard C, Lacroix C. Carbohydrates and the human gut microbiota. Curr Opin Clin Nutr Metab Care. 2013 Jul;16(4):453-60. doi: 10.1097/MCO.0b013e3283619e63. PMID: 23719143.
https://pubmed.ncbi.nlm.nih.gov/23719143
150d. Shade A, Handelsman J. Beyond the Venn diagram: the hunt for a core microbiome. Environ Microbiol. 2012 Jan;14(1):4-12. doi: 10.1111/j.1462-2920.2011.02585.x. Epub 2011 Oct 18. PMID: 22004523.
https://pubmed.ncbi.nlm.nih.gov/22004523
151. Mosca A, Leclerc M, Hugot JP. Gut Microbiota Diversity and Human Diseases: Should We Reintroduce Key Predators in Our Ecosystem? Front Microbiol. 2016 Mar 31;7:455. doi: 10.3389/fmicb.2016.00455. PMID: 27065999; PMCID: PMC4815357.
https://pubmed.ncbi.nlm.nih.gov/27065999
152. Caricilli AM, Saad MJ. Gut microbiota composition and its effects on obesity and insulin resistance. Curr Opin Clin Nutr Metab Care. 2014 Jul;17(4):312-8. doi: 10.1097/MCO.0000000000000067. PMID: 24848531.
https://pubmed.ncbi.nlm.nih.gov/24848531
153. Moeller AH, Li Y, Mpoudi Ngole E, Ahuka-Mundeke S, Lonsdorf EV, Pusey AE, Peeters M, Hahn BH, Ochman H. Rapid changes in the gut microbiome during human evolution. Proc Natl Acad Sci U S A. 2014 Nov 18;111(46):16431-5. doi: 10.1073/pnas.1419136111. Epub 2014 Nov 3. PMID: 25368157; PMCID: PMC4246287.
https://pubmed.ncbi.nlm.nih.gov/25368157
154. Adler CJ, Dobney K, Weyrich LS, Kaidonis J, Walker AW, Haak W, Bradshaw CJ, Townsend G, Sołtysiak A, Alt KW, Parkhill J, Cooper A. Sequencing ancient calcified dental plaque shows changes in oral microbiota with dietary shifts of the Neolithic and Industrial revolutions. Nat Genet. 2013 Apr;45(4):450-5, 455e1. doi: 10.1038/ng.2536. Epub 2013 Feb 17. PMID: 23416520; PMCID: PMC3996550.
https://pubmed.ncbi.nlm.nih.gov/23416520
155. Schnorr SL. The diverse microbiome of the hunter-gatherer. Nature. 2015 Feb 26;518(7540):S14-5. doi: 10.1038/518S14a. PMID: 25715276.
https://pubmed.ncbi.nlm.nih.gov/25715276
156. De Filippo C, Cavalieri D, Di Paola M, Ramazzotti M, Poullet JB, Massart S, Collini S, Pieraccini G, Lionetti P. Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. Proc Natl Acad Sci U S A. 2010 Aug 17;107(33):14691-6. doi: 10.1073/pnas.1005963107. Epub 2010 Aug 2. PMID: 20679230; PMCID: PMC2930426.
https://pubmed.ncbi.nlm.nih.gov/20679230
157. Lambrecht BN, Hammad H. The immunology of the allergy epidemic and the hygiene hypothesis. Nat Immunol. 2017 Sep 19;18(10):1076-1083. doi: 10.1038/ni.3829. PMID: 28926539.
https://pubmed.ncbi.nlm.nih.gov/28926539
158. Rook GA. 99th Dahlem conference on infection, inflammation and chronic inflammatory disorders: darwinian medicine and the ‘hygiene’ or ‘old friends’ hypothesis. Clin Exp Immunol. 2010 Apr;160(1):70-9. doi: 10.1111/j.1365-2249.2010.04133.x. PMID: 20415854; PMCID: PMC2841838.
https://pubmed.ncbi.nlm.nih.gov/20415854
159. Bloomfield SF, Rook GA, Scott EA, Shanahan F, Stanwell-Smith R, Turner P. Time to abandon the hygiene hypothesis: new perspectives on allergic disease, the human microbiome, infectious disease prevention and the role of targeted hygiene. Perspect Public Health. 2016 Jul;136(4):213-24. doi: 10.1177/1757913916650225. PMID: 27354505; PMCID: PMC4966430.
https://pubmed.ncbi.nlm.nih.gov/27354505
160. Moya A, Ferrer M. Functional Redundancy-Induced Stability of Gut Microbiota Subjected to Disturbance. Trends Microbiol. 2016 May;24(5):402-413. doi: 10.1016/j.tim.2016.02.002. Epub 2016 Mar 17. PMID: 26996765.
https://pubmed.ncbi.nlm.nih.gov/26996765
161. Ganu RS, Harris RA, Collins K, Aagaard KM. Early origins of adult disease: approaches for investigating the programmable epigenome in humans, nonhuman primates, and rodents. ILAR J. 2012;53(3-4):306-21. doi: 10.1093/ilar.53.3-4.306. PMID: 23744969; PMCID: PMC3747760.
https://pubmed.ncbi.nlm.nih.gov/23744969
162. Evenepoel P, Poesen R, Meijers B. The gut-kidney axis. Pediatr Nephrol. 2017 Nov;32(11):2005-2014. doi: 10.1007/s00467-016-3527-x. Epub 2016 Nov 15. PMID: 27848096.
https://pubmed.ncbi.nlm.nih.gov/27848096
163. Kennedy PJ, Cryan JF, Dinan TG, Clarke G. Kynurenine pathway metabolism and the microbiota-gut-brain axis. Neuropharmacology. 2017 Jan;112(Pt B):399-412. doi: 10.1016/j.neuropharm.2016.07.002. Epub 2016 Jul 5. PMID: 27392632.
https://pubmed.ncbi.nlm.nih.gov/27392632
164. Selber-Hnatiw S, Rukundo B, Ahmadi M, Akoubi H, Al-Bizri H, Aliu AF, Ambeaghen TU, Avetisyan L, Bahar I, Baird A, Begum F, Ben Soussan H, Blondeau-Éthier V, Bordaries R, Bramwell H, Briggs A, Bui R, Carnevale M, Chancharoen M, Chevassus T, Choi JH, Coulombe K, Couvrette F, D’Abreau S, Davies M, Desbiens MP, Di Maulo T, Di Paolo SA, Do Ponte S, Dos Santos Ribeiro P, Dubuc-Kanary LA, Duncan PK, Dupuis F, El-Nounou S, Eyangos CN, Ferguson NK, Flores-Chinchilla NR, Fotakis T, Gado Oumarou H D M, Georgiev M, Ghiassy S, Glibetic N, Grégoire Bouchard J, Hassan T, Huseen I, Ibuna Quilatan MF, Iozzo T, Islam S, Jaunky DB, Jeyasegaram A, Johnston MA, Kahler MR, Kaler K, Kamani C, Karimian Rad H, Konidis E, Konieczny F, Kurianowicz S, Lamothe P, Legros K, Leroux S, Li J, Lozano Rodriguez ME, Luponio-Yoffe S, Maalouf Y, Mantha J, McCormick M, Mondragon P, Narayana T, Neretin E, Nguyen TTT, Niu I, Nkemazem RB, O’Donovan M, Oueis M, Paquette S, Patel N, Pecsi E, Peters J, Pettorelli A, Poirier C, Pompa VR, Rajen H, Ralph RO, Rosales-Vasquez J, Rubinshtein D, Sakr S, Sebai MS, Serravalle L, Sidibe F, Sinnathurai A, Soho D, Sundarakrishnan A, Svistkova V, Ugbeye TE, Vasconcelos MS, Vincelli M, Voitovich O, Vrabel P, Wang L, Wasfi M, Zha CY, Gamberi C. Human Gut Microbiota: Toward an Ecology of Disease. Front Microbiol. 2017 Jul 17;8:1265. doi: 10.3389/fmicb.2017.01265. PMID: 28769880; PMCID: PMC5511848.
https://pubmed.ncbi.nlm.nih.gov/28769880
165. Lee YY, Hassan SA, Ismail IH, Chong SY, Raja Ali RA, Amin Nordin S, Lee WS, Majid NA. Gut microbiota in early life and its influence on health and disease: A position paper by the Malaysian Working Group on Gastrointestinal Health. J Paediatr Child Health. 2017 Dec;53(12):1152-1158. doi: 10.1111/jpc.13640. PMID: 29205651.
https://pubmed.ncbi.nlm.nih.gov/29205651
Glyphatic system
167. Jessen NA, Munk AS, Lundgaard I, Nedergaard M. The Glymphatic System: A Beginner’s Guide. Neurochem Res. 2015 Dec;40(12):2583-99. doi: 10.1007/s11064-015-1581-6. Epub 2015 May 7. PMID: 25947369; PMCID: PMC4636982.
https://pubmed.ncbi.nlm.nih.gov/25947369
168. Aspelund A, Antila S, Proulx ST, Karlsen TV, Karaman S, Detmar M, Wiig H, Alitalo K. A dural lymphatic vascular system that drains brain interstitial fluid and macromolecules. J Exp Med. 2015 Jun 29;212(7):991-9. doi: 10.1084/jem.20142290. Epub 2015 Jun 15. PMID: 26077718; PMCID: PMC4493418.
https://pubmed.ncbi.nlm.nih.gov/26077718
169. Sun BL, Wang LH, Yang T, Sun JY, Mao LL, Yang MF, Yuan H, Colvin RA, Yang XY. Lymphatic drainage system of the brain: A novel target for intervention of neurological diseases. Prog Neurobiol. 2018 Apr-May;163-164:118-143. doi: 10.1016/j.pneurobio.2017.08.007. Epub 2017 Sep 10. PMID: 28903061.
https://pubmed.ncbi.nlm.nih.gov/28903061
170. Natale G, Limanaqi F, Busceti CL, Mastroiacovo F, Nicoletti F, Puglisi-Allegra S, Fornai F. Glymphatic System as a Gateway to Connect Neurodegeneration From Periphery to CNS. Front Neurosci. 2021 Feb 9;15:639140. doi: 10.3389/fnins.2021.639140. PMID: 33633540; PMCID: PMC7900543.
https://pubmed.ncbi.nlm.nih.gov/33633540
171. Ma YY, Li X, Yu JT, Wang YJ. Therapeutics for neurodegenerative diseases by targeting the gut microbiome: from bench to bedside. Transl Neurodegener. 2024 Feb 27;13(1):12. doi: 10.1186/s40035-024-00404-1. PMID: 38414054; PMCID: PMC10898075.
https://pubmed.ncbi.nlm.nih.gov/38414054
172. Zhuang M, Zhang X, Cai J. Microbiota-gut-brain axis: interplay between microbiota, barrier function and lymphatic system. Gut Microbes. 2024 Jan-Dec;16(1):2387800. doi: 10.1080/19490976.2024.2387800. Epub 2024 Aug 25. PMID: 39182226; PMCID: PMC11346530.
https://pubmed.ncbi.nlm.nih.gov/39182226
Leaky gut
173. Fasano A. Leaky gut and autoimmune diseases. Clin Rev Allergy Immunol. 2012 Feb;42(1):71-8. doi: 10.1007/s12016-011-8291-x. PMID: 22109896.
https://pubmed.ncbi.nlm.nih.gov/22109896
174. Fasano A. Intestinal permeability and its regulation by zonulin: diagnostic and therapeutic implications. Clin Gastroenterol Hepatol. 2012 Oct;10(10):1096-100. doi: 10.1016/j.cgh.2012.08.012. Epub 2012 Aug 16. PMID: 22902773; PMCID: PMC3458511.
https://pubmed.ncbi.nlm.nih.gov/22902773
175. Barreau F, Hugot JP. Intestinal barrier dysfunction triggered by invasive bacteria. Curr Opin Microbiol. 2014 Feb;17:91-8. doi: 10.1016/j.mib.2013.12.003. Epub 2014 Jan 14. PMID: 24440560.
https://pubmed.ncbi.nlm.nih.gov/24440560
176. Caesar R, Fåk F, Bäckhed F. Effects of gut microbiota on obesity and atherosclerosis via modulation of inflammation and lipid metabolism. J Intern Med. 2010 Oct;268(4):320-8. doi: 10.1111/j.1365-2796.2010.02270.x. PMID: 21050286.
https://pubmed.ncbi.nlm.nih.gov/21050286
177. DaFonte TM, Valitutti F, Kenyon V, Locascio JJ, Montuori M, Francavilla R, Passaro T, Crocco M, Norsa L, Piemontese P, Baldassarre M, Fasano A, Leonard MM; CD-GEMM Study Group. Zonulin as a Biomarker for the Development of Celiac Disease. Pediatrics. 2024 Jan 1;153(1):e2023063050. doi: 10.1542/peds.2023-063050. PMID: 38062791; PMCID: PMC10754681.
https://pubmed.ncbi.nlm.nih.gov/38062791
Appetite of microbiome
178. Han H, Yi B, Zhong R, Wang M, Zhang S, Ma J, Yin Y, Yin J, Chen L, Zhang H. From gut microbiota to host appetite: gut microbiota-derived metabolites as key regulators. Microbiome. 2021 Jul 20;9(1):162. doi: 10.1186/s40168-021-01093-y. PMID: 34284827; PMCID: PMC8293578.
https://pubmed.ncbi.nlm.nih.gov/34284827
179. Dong Y, Dong J, Xiao H, Li Y, Wang B, Zhang S, Cui M. A gut microbial metabolite cocktail fights against obesity through modulating the gut microbiota and hepatic leptin signaling. J Sci Food Agric. 2024 Dec;104(15):9356-9367. doi: 10.1002/jsfa.13758. Epub 2024 Jul 19. PMID: 39030978.
https://pubmed.ncbi.nlm.nih.gov/39030978
180. Li S, Liu M, Han Y, Liu C, Cao S, Cui Y, Zhu X, Wang Z, Liu B, Shi Y. Gut microbiota-derived gamma-aminobutyric acid improves host appetite by inhibiting satiety hormone secretion. mSystems. 2024 Oct 22;9(10):e0101524. doi: 10.1128/msystems.01015-24. Epub 2024 Sep 24. PMID: 39315776; PMCID: PMC11495008.
https://pubmed.ncbi.nlm.nih.gov/39315776
181. Wang Z, Yang S, Liu L, Mao A, Kan H, Yu F, Ma X, Feng L, Zhou T. The gut microbiota-derived metabolite indole-3-propionic acid enhances leptin sensitivity by targeting STAT3 against diet-induced obesity. Clin Transl Med. 2024 Dec;14(12):e70053. doi: 10.1002/ctm2.70053. PMID: 39606796; PMCID: PMC11602751.
https://pubmed.ncbi.nlm.nih.gov/39606796
182. Tan S, Santolaya JL, Wright TF, Liu Q, Fujikawa T, Chi S, Bergstrom CP, Lopez A, Chen Q, Vale G, McDonald JG, Schmidt A, Vo N, Kim J, Baniasadi H, Li L, Zhu G, He TC, Zhan X, Obata Y, Jin A, Jia D, Elmquist JK, Sifuentes-Dominguez L, Burstein E. Interaction between the gut microbiota and colonic enteroendocrine cells regulates host metabolism. Nat Metab. 2024 Jun;6(6):1076-1091. doi: 10.1038/s42255-024-01044-5. Epub 2024 May 22. PMID: 38777856.
https://pubmed.ncbi.nlm.nih.gov/38777856
183. Grifka-Walk HM, Jenkins BR, Kominsky DJ. Amino Acid Trp: The Far Out Impacts of Host and Commensal Tryptophan Metabolism. Front Immunol. 2021 Jun 4;12:653208. doi: 10.3389/fimmu.2021.653208. PMID: 34149693; PMCID: PMC8213022.
https://pubmed.ncbi.nlm.nih.gov/34149693
184. Ringseis R, Gessner DK, Eder K. The Gut-Liver Axis in the Control of Energy Metabolism and Food Intake in Animals. Annu Rev Anim Biosci. 2020 Feb 15;8:295-319. doi: 10.1146/annurev-animal-021419-083852. Epub 2019 Nov 5. PMID: 31689373.
https://pubmed.ncbi.nlm.nih.gov/31689373
185. Ribeiro G, Schellekens H, Cuesta-Marti C, Maneschy I, Ismael S, Cuevas-Sierra A, Martínez JA, Silvestre MP, Marques C, Moreira-Rosário A, Faria A, Moreno LA, Calhau C. A Menu for Microbes: Unraveling Appetite Regulation and Weight Dynamics Through the Microbiota-Brain Connection Across the Lifespan. Am J Physiol Gastrointest Liver Physiol. 2025 Jan 15. doi: 10.1152/ajpgi.00227.2024. Epub ahead of print. PMID: 39811913.
https://pubmed.ncbi.nlm.nih.gov/39811913
186. Holliday A, Horner K, Johnson KO, Dagbasi A, Crabtree DR. Appetite-related Gut Hormone Responses to Feeding Across the Life Course. J Endocr Soc. 2025 Jan 6;9(2):bvae223. doi: 10.1210/jendso/bvae223. PMID: 39777204; PMCID: PMC11702868.
https://pubmed.ncbi.nlm.nih.gov/39777204
187. Yang K, Wu YT, He Y, Dai JX, Luo YL, Xie JH, Ding WJ. GLP-1 and IL-6 regulates obesity in the gut and brain. Life Sci. 2025 Feb 1;362:123339. doi: 10.1016/j.lfs.2024.123339. Epub 2024 Dec 25. PMID: 39730038.
https://pubmed.ncbi.nlm.nih.gov/39730038
188. Chimera B, Hoobler R, Deschasaux-Tanguy M, Van Merris E, Roels O, Playdon M, Michels N, Huybrechts I. The gut microbiome and eating behavior outcomes: A systematic review. Obes Rev. 2024 Dec 12:e13880. doi: 10.1111/obr.13880. Epub ahead of print. PMID: 39667924.
https://pubmed.ncbi.nlm.nih.gov/39667924
189. Niu Y, Yu W, Kou X, Wu S, Liu M, Chen C, Ji J, Shao Y, Xue Z. Bioactive compounds regulate appetite through the melanocortin system: a review. Food Funct. 2024 Dec 9;15(24):11811-11833. doi: 10.1039/d4fo04024d. PMID: 39506527.
https://pubmed.ncbi.nlm.nih.gov/39506527
190. Yu M, Yu B, Chen D. The effects of gut microbiota on appetite regulation and the underlying mechanisms. Gut Microbes. 2024 Jan-Dec;16(1):2414796. doi: 10.1080/19490976.2024.2414796. Epub 2024 Nov 6. PMID: 39501848; PMCID: PMC11542600.
https://pubmed.ncbi.nlm.nih.gov/39501848
191. Breton J, Jacquemot J, Yaker L, Leclerc C, Connil N, Feuilloley M, Déchelotte P, Fetissov SO. Host Starvation and Female Sex Influence Enterobacterial ClpB Production: A Possible Link to the Etiology of Eating Disorders. Microorganisms. 2020 Apr 7;8(4):530. doi: 10.3390/microorganisms8040530. PMID: 32272706; PMCID: PMC7232239.
https://pubmed.ncbi.nlm.nih.gov/32272706
192. Romaní-Pérez M, Bullich-Vilarrubias C, López-Almela I, Liébana-García R, Olivares M, Sanz Y. The Microbiota and the Gut-Brain Axis in Controlling Food Intake and Energy Homeostasis. Int J Mol Sci. 2021 May 29;22(11):5830. doi: 10.3390/ijms22115830. PMID: 34072450; PMCID: PMC8198395.
MMV maakt wekelijks een selectie uit het nieuws over voeding en leefstijl in relatie tot kanker en andere medische condities.
Inschrijven nieuwsbrief








